Rheumatoid arthritis (RA) is a chronic systemic inflammatory autoimmune disorder characterized by deforming symmetrical polyarthritis of varying extent and severity. It is associated with synovitis of joint and tendon sheaths, articular cartilage loss, erosion of juxta-articular bone, and the presence of IgM rheumatoid factor in the blood in most patients.1 In some patients, systemic and extra-articular features may be observed during the disease and rarely before the joint disease. These include anaemia, weight loss, vasculitis, serositis, interstitial inflammation in lungs and exocrine, salivary, and lacrimal glands, as well as nodules in subcutaneous, pulmonary, and scleral tissues.2
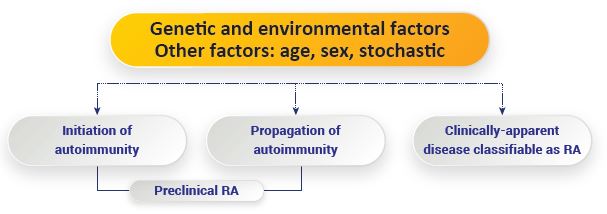
RA is the most common inflammatory arthritis, affecting approximately 0.1-2% of the adult population worldwide. It is responsible for around 250,000 hospitalizations and 9 million physician visits every year. The onset of RA usually occurs between 30 to 50 years of age and is 2-3 times more likely to occur in women than men.3 In India, studies have confirmed the prevalence rate to be between 0.28- 0.7%.4 Leti untreated, about 20-30% of RA patients become permanently work-disabled within 3-4 years of diagnosis. One of the forecasts suggests that the rate of practioner-diagnosed arthritis will increase by almost 49% by 2040 due to the worldwide ageing population.Genetic and environmental factors play a major role in the development and progression of RA. Almost 55-60% of RA is from genetic factors. Around 60 genetic loci exist associated with susceptibility of RA across multiple populations.5 Changes in the synovial fluid of patients with RA seem to increase the pro-inflammatory cytokines. Other factors may include lifestyle choices, diet preferences, age, sex, and toxic exposures that trigger the onset or progression of the disease.6
A major advance in how factors influence the development of RA, especially seropositive RA, often involves increased production of antibodies that are detectable more than 5-10 years before RA can be diagnosed. This period can be termed as the ‘Preclinical Phase.’ In one study of patients with musculoskeletal complaints, patients with the highest levels of antibodies at baseline were at a 62% increased likelihood to be diagnosed with RA at five years.7

Currently, two concepts predominantly guide early RA treatment.
1. Aggressive therapy
2. Treat to Target therapy
Early aggressive therapy uses medications to reduce inflammation and prevent joint destruction that may lead to pain and disability. Treat to target therapy is focused on treating the target i.e., the disease activity.8
The first-line therapy for RA treatment includes the use of NSAIDs and corticosteroids. Fast-acting NSAIDs inhibit cyclooxygenase from preventing prostaglandins, prostacyclin, and thromboxane synthesis. On the other hand, corticosteroids are more potent, anti-inflammatory agents that prevent the release of phospholipids and decrease the effects of eosinophils, thereby reducing inflammation. The drawback of using these agents, however, is their side-effect profiles.9
The second-line therapy for RA includes the Disease-modifying anti-rheumatic drugs (DMARDs) that promote remission or slow/stop the progression of joint destruction and deformity. These agents have been shown to reduce the risk of developing lymphoma associated with RA. Methotrexate (MTX) is the first-choice second-line drug. It is an immunosuppressive and analogue of folic acid that impairs the metabolism of purines and pyrimidines and blocks the synthesis of amino acids and polyamines.10
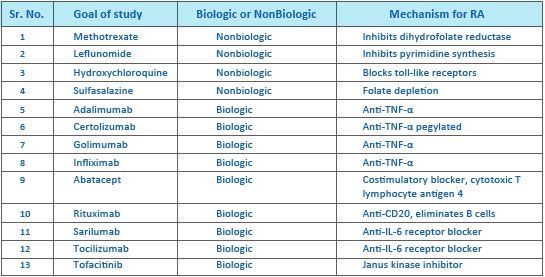
Joint surgery in patients with RA is usually the last resort for the treatment of RA. The goal of surgical procedures in the management of RA is primarily to reduce joint pain and restore the functions of the joints and improve quality of life.
A wide range of non-pharmacologic treatment and management options are available in the current day and age. The aim is to improve and amplify joint movement, muscle strength, the performance of day-to-day activities with ease, and to improve the quality of life (QOL) of patients suffering due to RA. These treatment options also help reduce the impact of the disease and related comorbidities. Patient education and counselling are central to the
management of RA.

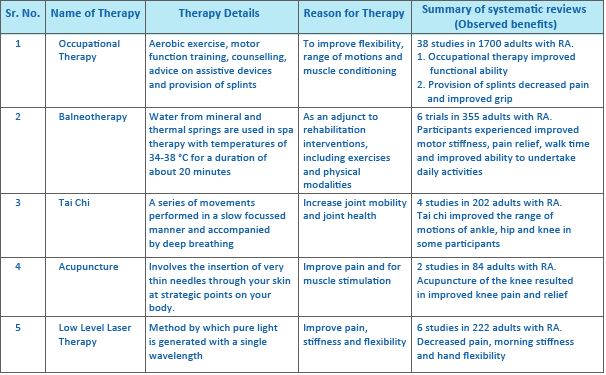
Other non-pharmacologic therapies include thermotherapy to improve stiffness and relieve pain, joint protection, and energy conservation techniques like aids, devices, and adaptations to the physical environment, use of orthoses underpinned to a patient’s body to align, support, and improve function. Special shoes and inserts are also used to reduce shock and provide further support. Cognitive behavioural therapies are also developed to target the mood of the patient’s suffering due to RA. It is a structured self-management intervention that teaches a blend of cognitive and behavioural management.12
Omega-3 fatty acids may be protective and reduce the risk of RA.13 A healthy eating pattern that includes whole grains, fruits, and vegetables has also been correlated with a decreased diagnosis. Curcumin has also been suggested as a supplement that may not only reduce inflammation in RA patients but may also help manage the P. gingivalis infection seen in so many of these patients.14
Rheumatoid arthritis is a disease that affects many people and has a debilitating effect on the quality of life. New advances in rheumatoid arthritis treatment are constantly being made. Both pharmacological, and non-pharmacological therapies have shown to be effective in the treatment and management of rheumatoid arthritis.
References:
1. Yap, H., Tee, S., Wong, M., Chow, S., Peh, S. and Teow, S., 2022. Pathogenic Role of Immune Cells in Rheumatoid Arthritis: Implications in Clinical Treatment and Biomarker Development.
2. Wasserman, A., 2018. Rheumatoid Arthritis: Common Questions About Diagnosis and Management. American Family Physician, 97(7), pp.455-462.
3. Almutairi, K., Nossent, J., Preen, D., Keen, H. and Inderjeeth, C., 2020. The global prevalence of rheumatoid arthritis: a meta-analysis based on a systematic review. Rheumatology International, 41(5), pp.863-877.
4. Handa, R., Rao, U., Lewis, J., Rambhad, G., Shiff, S. and Ghia, C., 2015. Literature review of rheumatoid arthritis in India. International Journal of Rheumatic Diseases, 19(5), pp.440-451.
5. Rindfleisch, A., 2005. Diagnosis and Management of Rheumatoid Arthritis. American Family Physician, 72(6), pp.1037-1047.
6. Deane, K., Demoruelle, M., Kelmenson, L., Kuhn, K., Norris, J. and Holers, V., 2017. Genetic and environmental risk factors for rheumatoid arthritis. Best Practice & Research Clinical Rheumatology, 31(1), pp.3-18.
7. Rakieh, C., Nam, J., Hunt, L., Hensor, E., Das, S., Bissell, L., Villeneuve, E., McGonagle, D., Hodgson, R., Grainger, A., Wakefield, R., Conaghan, P. and Emery, P., 2022. Predicting the development of clinical arthritis in anti-CCP positive individuals with non-specific musculoskeletal symptoms: a prospective observational cohort study
8. PV, A. and AR, S., 2022. A NOVEL APPROACH IN PATIENT CARE AND NON-PHARMACOLOGICAL TREATMENT FOR RHEUMATOID ARTHRITIS..
9. Bullock, J., Rizvi, S., Saleh, A., Ahmed, S., Do, D., Ansari, R. and Ahmed, J., 2018. Rheumatoid Arthritis: A Brief Overview of the Treatment. Medical Principles and Practice, 27(6), pp.501-507.
10. Smolen, J., Landewé, R., Breedveld, F., et al., 2010. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs. Annals of the Rheumatic Diseases, 69(6), pp.964-975.
11. Shaw, K., 2007. Nonpharmacological interventions for rheumatoid arthritis. Australian Family Physicians, 36(10).
12. Küçükdeveci, A., 2019. Nonpharmacological treatment in established rheumatoid arthritis. Best Practice & Research Clinical Rheumatology, 33(5), p.101482.
13. He, J., Wang, Y., Feng, M., et al., 2016. Dietary intake and risk of rheumatoid arthritis—a cross section multicenter study. Clinical Rheumatology, 35(12), pp.2901-2908. 14. Asteriou, E., Gkoutzourelas, A., Mavropoulos, A., Katsiari, C., Sakkas, L. and Bogdanos, D., 2018. Curcumin for the Management of Periodontitis and Early ACPA-Positive Rheumatoid Arthritis: Killing Two Birds with One Stone. Nutrients, 10(7), p.908.
